I spent the better part of a decade telling clients that probiotics were primarily a digestive tool, good for bloating, good for regularity, maybe helpful after a round of antibiotics. Then, around 2021, I started reading the psychobiotics research coming out of Ireland and Japan, and I realized I had been thinking about an entire category of supplements with one eye closed. The clinical data linking specific probiotic strains to measurable reductions in anxiety and depressive symptoms is no longer preliminary. In 2026, it is substantial, replicated, and increasingly difficult to dismiss.
But here is the problem. The supplement aisle does not make this easy. Walk into any health food store and you will find dozens of probiotic products, most of them marketed with vague promises about “gut health” or “immune support.” Very few disclose the specific strain designations that actually matter for mood. And almost none cite the human clinical trials that separate genuine psychobiotics from expensive placebos.
This guide is designed to cut through that noise. If you have been reading about the science behind the gut-brain connection and want to know which probiotics have real evidence for anxiety and depression, this is where the details live.
What makes a probiotic a “psychobiotic”?
The term psychobiotic was coined in 2013 by Ted Dinan and John Cryan at University College Cork, two researchers who have done more than almost anyone to legitimize the gut-brain axis in mainstream psychiatry. They defined psychobiotics as live organisms that, when ingested in adequate amounts, produce a health benefit in patients suffering from psychiatric illness.
That definition has since expanded. Today, the psychobiotics category includes both specific probiotic strains and prebiotics that influence brain function through the gut microbiome. But the core principle remains: not every probiotic qualifies. The strain has to demonstrate a neurological or psychological benefit in controlled human studies, not just in mice, not just in petri dishes.
This distinction matters because the probiotic industry is enormous and loosely regulated. A product can legally call itself a “mood support probiotic” without a single clinical trial behind it. The strains listed below have earned their reputation through published, peer-reviewed research.
The strains with the strongest evidence
After reviewing the literature extensively and tracking which strains consistently appear in meta-analyses, three stand out above the rest for anxiety and depression.
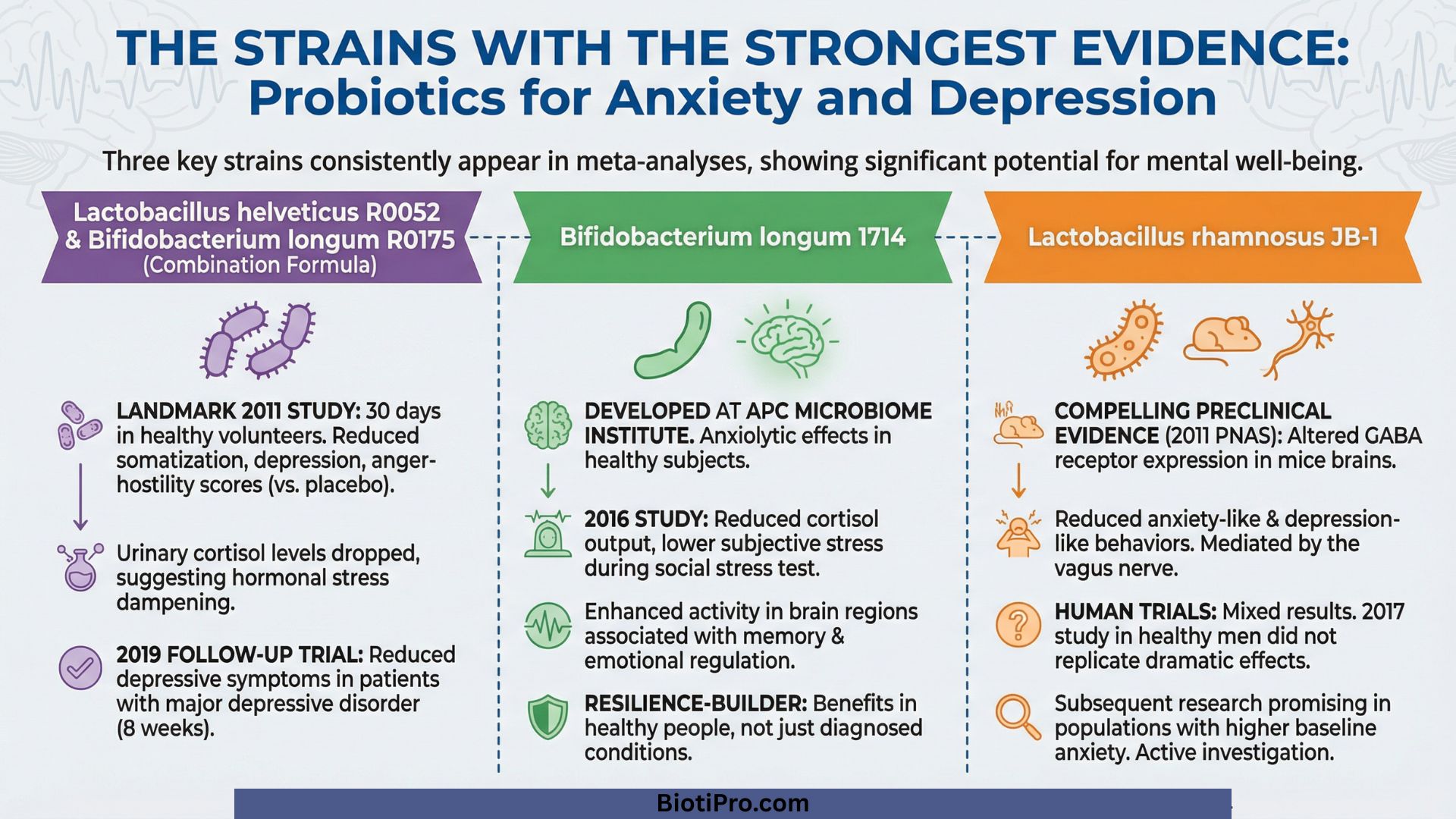
Lactobacillus helveticus R0052 and Bifidobacterium longum R0175
These two strains are often studied together as a combination formula. A landmark 2011 study in the British Journal of Nutrition gave this combination to healthy volunteers for 30 days and measured psychological distress using validated scales. The probiotic group showed significant reductions in somatization, depression, and anger-hostility scores compared to placebo. Urinary cortisol levels also dropped, suggesting a genuine dampening of the stress response at the hormonal level.
Since then, multiple follow-up trials have confirmed these findings. A 2019 randomized controlled trial in Nutrients found that the same combination reduced depressive symptoms in patients with diagnosed major depressive disorder over eight weeks.
Bifidobacterium longum 1714
This strain, developed at the APC Microbiome Institute, has demonstrated anxiolytic effects in healthy human subjects. A 2016 study in Translational Psychiatry showed that participants taking B. longum 1714 for four weeks had reduced cortisol output and reported lower subjective stress levels when exposed to a standardized social stress test. EEG measurements also showed enhanced activity in brain regions associated with memory and emotional regulation.
What makes this strain particularly interesting is that the benefits appeared in healthy people, not just those with diagnosed conditions. That suggests B. longum 1714 may function as a resilience-builder, not just a treatment.
Lactobacillus rhamnosus JB-1
The preclinical evidence for this strain is among the most compelling in the field. In a widely cited 2011 study published in PNAS, researchers at McMaster University showed that L. rhamnosus JB-1 altered GABA receptor expression across multiple brain regions in mice and reduced anxiety-like and depression-like behaviors. The effect was mediated by the vagus nerve. When the vagus nerve was severed, the benefits disappeared entirely.
Human trials with this strain have produced mixed results, which is worth acknowledging honestly. A 2017 study in healthy men did not replicate the dramatic effects seen in mice. However, subsequent research in populations with higher baseline anxiety has shown more promising outcomes. The strain remains under active investigation.
Strain comparison at a glance
| Strain | Primary Benefit | Key Study | Evidence Level |
| L. helveticus R0052 + B. longum R0175 | Reduced depression, lower cortisol | Messaoudi et al., 2011 (Br J Nutr) | Strong (multiple RCTs) |
| B. longum 1714 | Lower stress reactivity, improved emotional processing | Allen et al., 2016 (Transl Psychiatry) | Moderate-Strong (healthy + clinical) |
| L. rhamnosus JB-1 | GABA modulation, anxiolytic effects | Bravo et al., 2011 (PNAS) | Strong preclinical, mixed human |
| L. plantarum PS128 | Dopamine/serotonin modulation | Liu et al., 2019 (Nutrients) | Emerging (promising RCTs) |
| L. casei Shirota | Reduced anxiety in chronic fatigue | Rao et al., 2009 (Gut Pathogens) | Moderate |
One strain worth watching is Lactobacillus plantarum PS128, sometimes called a “neurobiotic.” Research out of National Yang Ming University in Taiwan has shown it modulates dopamine and serotonin pathways, with clinical trials underway for autism spectrum and Parkinson’s-related mood symptoms.
How to read a probiotic label for mood support
Most consumers look at one number on a probiotic label: the CFU count. Billions of CFUs sound impressive, and marketing departments know it. But CFU count is almost irrelevant if the strains inside the capsule have no evidence for the benefit you are seeking.
Here is what actually matters when choosing a probiotic for anxiety or depression.
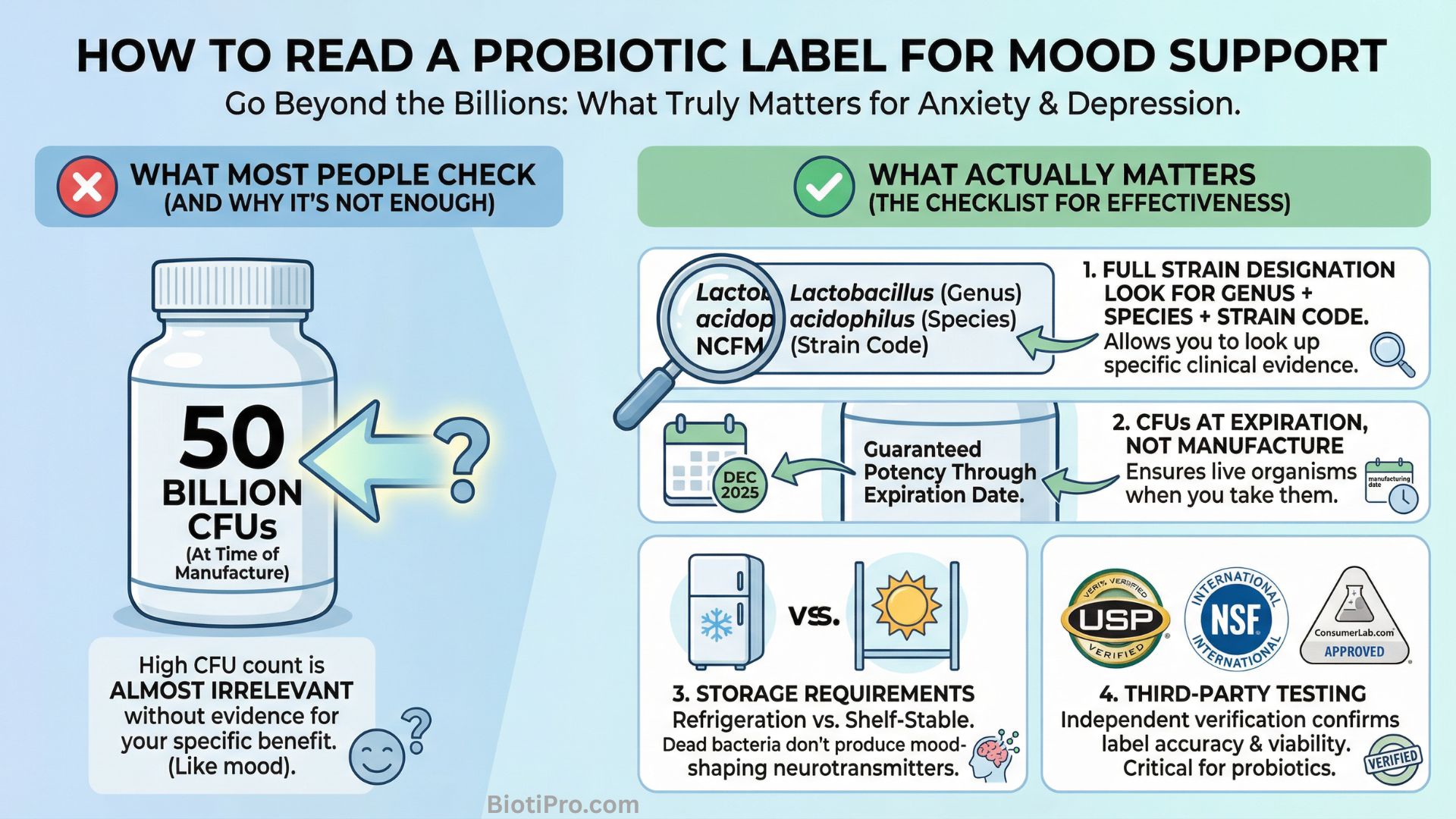
Full strain designation. The label should list genus, species, and strain. “Lactobacillus acidophilus” tells you almost nothing. “Lactobacillus acidophilus NCFM” tells you exactly which organism you are getting and allows you to look up its specific clinical evidence. If a product lists only genus and species without the strain code, consider that a red flag.
Colony-forming units at expiration, not at manufacture. Some products guarantee CFU counts at the time of manufacturing, which means the number of live organisms may have declined significantly by the time you take them. Look for products that guarantee potency through the expiration date.
Storage requirements. Some strains require refrigeration. Others are shelf-stable. Neither is inherently better, but you need to know which type you have and store it accordingly. Dead bacteria do not produce neurotransmitters that shape your mood.
Third-party testing. Independent verification from organizations like USP, NSF International, or ConsumerLab confirms that what is on the label is actually in the product. This matters more in the probiotic category than almost any other supplement category because viability is difficult for consumers to verify on their own.
What probiotics cannot do (and why that matters)
I want to be direct about this because the wellness space often is not. Probiotics are not antidepressants. They are not a substitute for therapy, medication, or professional psychiatric care. The effect sizes seen in clinical trials are real but modest, generally comparable to the lower end of what conventional antidepressants achieve in mild to moderate depression.
Where psychobiotics appear most promising is as a complementary strategy. Someone already working with a mental health professional, eating a nutrient-dense diet, managing stress, and sleeping adequately may find that adding a clinically supported probiotic strain provides an additional, meaningful layer of support. Someone relying on probiotics alone to manage severe depression is likely to be disappointed.
The other caveat is timeline. Unlike a pharmaceutical anxiolytic, which can take effect within hours, probiotics need time to colonize, interact with the existing microbiome, and shift metabolic output. Most clinical trials run for a minimum of four weeks before measuring outcomes, and many show stronger effects at the eight-week mark. Patience is part of the protocol.
The bigger picture: food first, supplements second
The most effective approach to supporting your gut-brain axis through beneficial bacteria is not a capsule. It is a dietary pattern. Fermented foods deliver live microorganisms in a complex food matrix that supports colonization and diversity in ways that isolated supplement strains cannot fully replicate. Prebiotic fibers fuel the bacteria already living in your gut. And dietary diversity ensures that no single microbial population dominates at the expense of others.
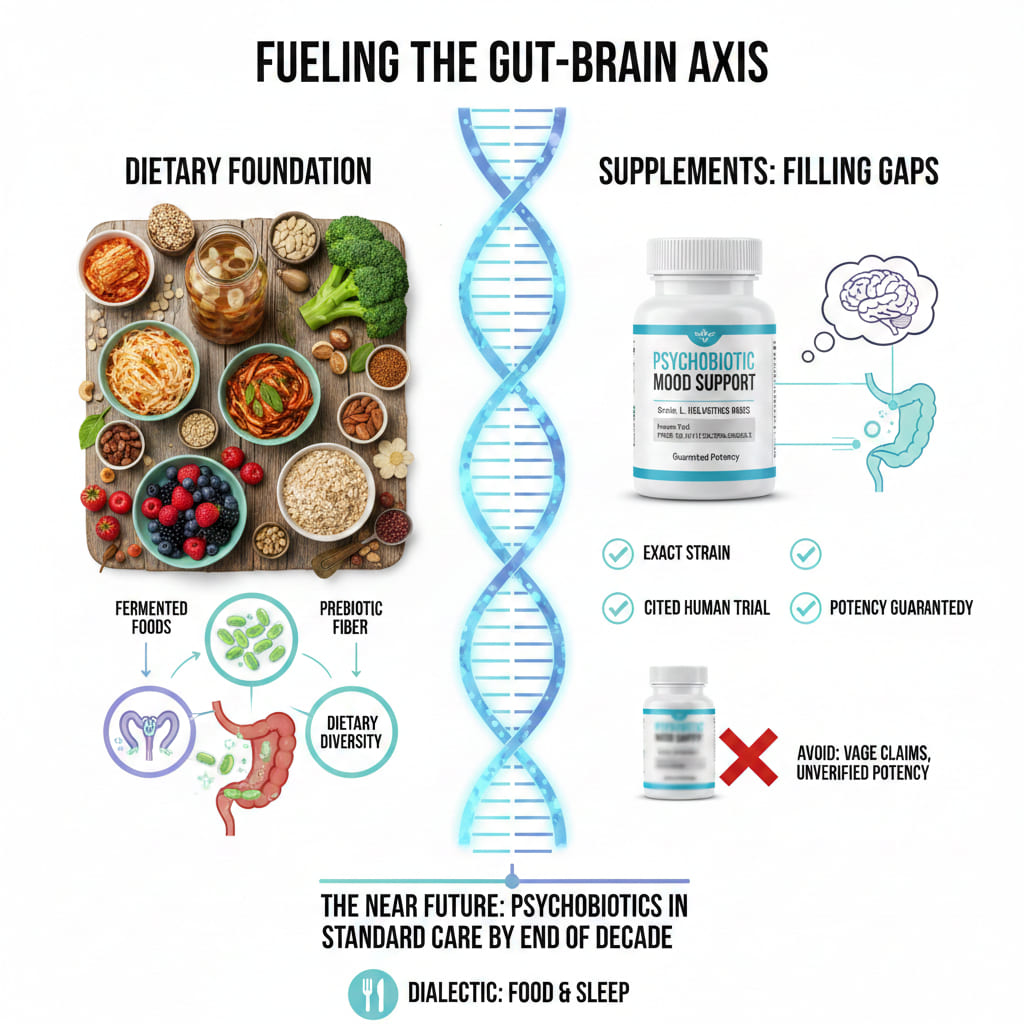
Supplements fill gaps. They can introduce specific strains with targeted evidence for mood support. But they work best when layered on top of a foundation that already prioritizes microbial health through whole foods, fiber, and fermentation.
The research trajectory is clear: by the end of this decade, psychobiotics will almost certainly be integrated into standard psychiatric care protocols, prescribed alongside or even instead of certain medications for mild mood disorders. We are not there yet. But we are closer than most people think.
If you are standing in the supplement aisle right now, staring at 40 different probiotic bottles with 40 different marketing claims, ask yourself one question: does this product name the exact strain, cite a human trial, and guarantee potency through expiration? If the answer to all three is yes, you might be holding something worth trying. If the answer to any of them is no, put it back and keep looking. And while you are rethinking what goes into your gut, it is worth considering whether what you eat for dinner tonight could also reshape how you sleep.