Three days without a bowel movement used to be unthinkable. Now it has become your new normal. You are bloated, uncomfortable, and wondering if something is seriously wrong or if this is just another price to pay for the weight loss everyone keeps complimenting.
Constipation ranks among the top three complaints from GLP-1 medication users, affecting up to 24% of patients in clinical trials. The combination of dramatically reduced food volume, slowed gastric motility, and inadequate fiber creates a perfect storm for digestive misery. Yet the solution is not as simple as loading up on fiber supplements. Done wrong, increasing fiber can make symptoms significantly worse. Managing these side effects successfully requires understanding how GLP-1 medications affect your entire digestive system, the complete guide to GLP-1 nutrition covers the full picture, including how to structure your diet to minimize gut disruption from the start of treatment.
Understanding how fiber works within the context of GLP-1 therapy transforms gut health from a frustrating side effect into a manageable component of treatment.
GLP-1 receptor agonists are a class of injectable medications originally developed to treat type 2 diabetes. They mimic glucagon-like peptide-1, a natural hormone that regulates blood sugar, slows gastric emptying, and signals fullness to the brain.
Because they significantly reduce appetite, several GLP-1 medications are now FDA-approved for chronic weight management in adults with obesity or overweight with related health conditions.
Common examples: Ozempic and Wegovy (semaglutide), Mounjaro and Zepbound (tirzepatide), Saxenda (liraglutide), and Trulicity (dulaglutide).
Why constipation becomes so common on GLP-1s
GLP-1 receptor agonists slow everything down. That is part of how they work. By delaying gastric emptying, these medications keep food in your stomach longer, prolonging satiety signals and reducing appetite. But the slowing effect does not stop at the stomach.
The entire gastrointestinal tract moves more sluggishly during GLP-1 therapy. Transit time from eating to elimination lengthens. Stool sits in the colon longer, allowing more water to be reabsorbed. The result is harder, drier stool that becomes increasingly difficult to pass.
Reduced food intake compounds the problem. Bulk matters for bowel function. The physical volume of food moving through your digestive system stimulates peristalsis, the wave-like muscle contractions that propel contents forward. Eat dramatically less food and you remove a key mechanical stimulus for regular bowel movements.
Dehydration adds another layer. Many GLP-1 users report diminished thirst alongside reduced hunger. Fluid intake drops without conscious awareness. Less water in the system means less water available to keep stool soft and passable.
Finally, the foods GLP-1 users tend to tolerate best often provide minimal fiber. Bland proteins, simple carbohydrates, and smooth textures go down easier when nausea lurks. Vegetables, whole grains, and legumes, the fiber powerhouses, frequently get pushed aside.
The two types of fiber and why it matters
Not all fiber behaves the same way in your digestive system. Understanding the distinction between soluble and insoluble fiber helps explain why some fiber strategies help constipation while others worsen bloating and discomfort.
Soluble fiber dissolves in water to form a gel-like substance. It softens stool, feeds beneficial gut bacteria, and tends to be gentler on sensitive digestive systems. Sources include oats, barley, psyllium husk, chia seeds, flaxseeds, apples, citrus fruits, and legumes.
Insoluble fiber does not dissolve in water. It adds bulk to stool and speeds transit time by physically stimulating the intestinal walls. Sources include wheat bran, whole wheat products, vegetables, nuts, and the skins of fruits.
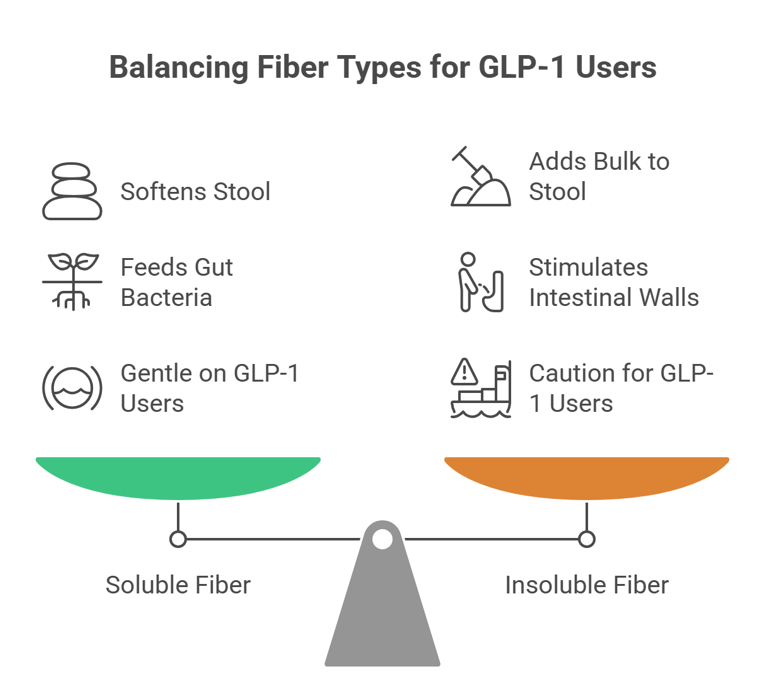
For GLP-1 users already dealing with slowed motility and reduced food volume, the approach to these fiber types requires nuance.
Soluble fiber generally works well during GLP-1 therapy. Its gentle, water-attracting properties help soften stool without adding excessive bulk that could worsen feelings of fullness or bloating. Psyllium husk in particular has strong evidence for relieving constipation while remaining well-tolerated.
Insoluble fiber requires more caution. Large amounts of wheat bran or raw vegetables in a gut already moving slowly can create backup rather than relief. The bulk sits there, potentially increasing bloating and discomfort before eventually clearing.
The ideal approach for most GLP-1 users emphasizes soluble fiber while including moderate amounts of insoluble fiber as tolerated.
How much fiber do GLP-1 users need?
Standard recommendations suggest 25 to 30 grams of fiber daily for adults. Most Americans consume roughly half that amount even without appetite-suppressing medications. GLP-1 users often consume far less.
Hitting 25 grams of fiber while eating 1,000 to 1,200 calories daily requires extraordinary intentionality. Every eating occasion must include fiber-rich foods. Supplementation often becomes necessary to bridge the gap.
A realistic target for most GLP-1 users falls in the 20 to 25 gram range, with emphasis on reaching at least 15 grams even on difficult days. This amount provides meaningful digestive benefits without requiring food volumes that reduced appetite cannot accommodate.
The key is gradual progression. Jumping from 8 grams daily to 25 grams overnight guarantees bloating, gas, and cramping. Increase fiber intake by 3 to 5 grams every few days, allowing your gut microbiome time to adapt to the changing substrate.
High-fiber foods that work for GLP-1 users
Selecting fiber sources that provide maximum benefit per bite matters enormously when total food intake is limited. These options deliver substantial fiber in manageable portions that most GLP-1 users tolerate well.
| Food | Serving Size | Fiber (grams) | Notes |
| Chia seeds | 2 tablespoons | 10 | Mostly soluble, add to yogurt or smoothies |
| Psyllium husk | 1 tablespoon | 7 | Pure soluble fiber, mix with water |
| Raspberries | 1 cup | 8 | High fiber-to-sugar ratio |
| Avocado | 1/2 medium | 5 | Also provides healthy fats |
| Lentils | 1/2 cup cooked | 8 | Excellent protein-fiber combo |
| Black beans | 1/2 cup | 7.5 | Rinse canned beans to reduce gas |
| Artichoke hearts | 1/2 cup | 7 | Mild flavor, easy to add to dishes |
| Pear | 1 medium | 5.5 | Eat with skin for full benefit |
| Oatmeal | 1 cup cooked | 4 | Soluble fiber, gentle on stomach |
| Ground flaxseed | 2 tablespoons | 4 | Add to smoothies, yogurt, baked goods |
Chia seeds deserve special mention for GLP-1 users. Two tablespoons deliver 10 grams of fiber, primarily soluble, in a format that can be stirred into Greek yogurt, blended into protein shakes, or soaked overnight to create a pudding. This single addition can transform fiber intake without requiring significant additional food volume.
Strategic fiber supplementation
When whole food fiber falls short, supplements provide a practical bridge. The supplement market offers numerous options with varying mechanisms and tolerability profiles.
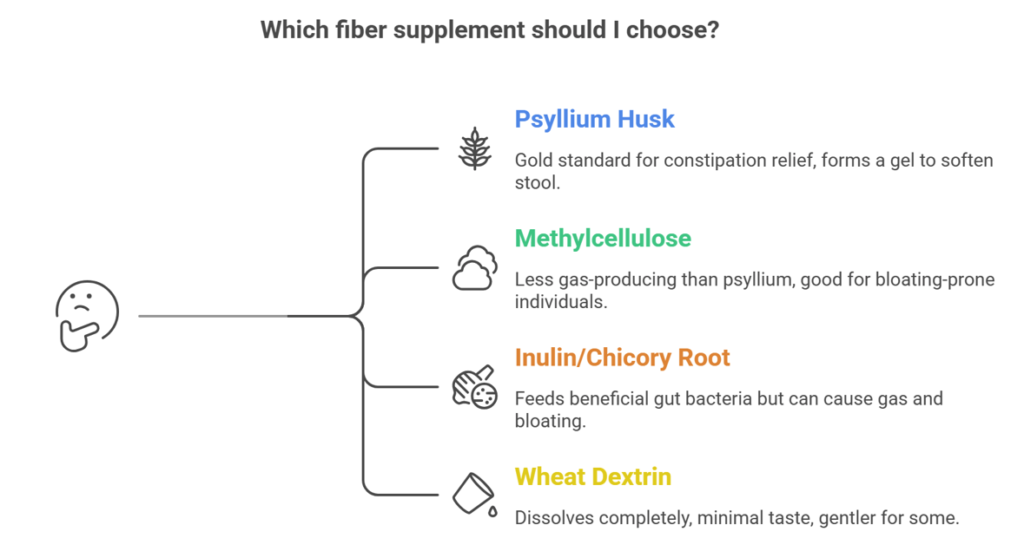
Psyllium husk (Metamucil, Konsyl) remains the gold standard for constipation relief. This pure soluble fiber forms a gel that softens stool and promotes regular bowel movements. Start with half the recommended dose and increase gradually. Take with a full glass of water to prevent the fiber from gelling in your throat or causing obstruction.
Methylcellulose (Citrucel) offers another soluble fiber option that many users find less gas-producing than psyllium. It does not ferment in the colon as readily, making it a good choice for those prone to bloating.
Inulin and chicory root fiber appear in many prebiotic supplements and fiber-fortified foods. These fermentable fibers feed beneficial gut bacteria but can cause significant gas and bloating, especially when introduced quickly. Use cautiously during GLP-1 therapy.
Wheat dextrin (Benefiber) dissolves completely in liquid and has minimal taste. It provides soluble fiber without the thickness of psyllium. Some users find it gentler, though evidence for constipation relief is less robust than psyllium.
Timing fiber supplements appropriately matters. Taking fiber too close to meals can increase feelings of fullness and reduce already-limited food intake. Many users find taking fiber supplements between meals or before bed works best.
Beyond fiber: a complete gut health strategy
Fiber alone does not solve all digestive complaints during GLP-1 therapy. A comprehensive approach addresses multiple factors contributing to gut dysfunction.

Hydration cannot be overemphasized. Fiber without adequate water creates a concrete-like mass in your intestines rather than soft, passable stool. Aim for a minimum of 64 ounces of fluid daily, more if you are increasing fiber intake or experiencing hot weather or exercise. Water, herbal tea, and broth all count.
Movement stimulates gut motility. Even gentle walking helps propel contents through the digestive system. A 15-minute walk after meals can meaningfully improve transit time. More vigorous exercise provides additional benefit but is not required for basic digestive function.
Probiotics support the gut microbiome, which is adapting to changes in substrate availability as your diet shifts. Research on specific strains for constipation shows promise for Bifidobacterium lactis and certain Lactobacillus species. Probiotic-rich foods like yogurt, kefir, and sauerkraut provide natural sources alongside or instead of supplements.
Magnesium serves double duty as both a commonly deficient mineral and a natural stool softener. Magnesium citrate and magnesium oxide have the strongest laxative effects. Magnesium glycinate is gentler but still supports bowel regularity while providing better absorption for addressing deficiency.
Timing and consistency matter more than any single intervention. Regular meal times, even when eating small amounts, help establish predictable digestive patterns. The gut responds to routine.
When to seek medical attention
Most constipation during GLP-1 therapy resolves with dietary adjustments and lifestyle modifications. However, certain warning signs warrant medical evaluation.
Seek attention if you experience complete absence of bowel movements for more than a week, severe abdominal pain, vomiting, blood in stool, or signs of intestinal obstruction such as inability to pass gas combined with progressive abdominal distension.
Chronic constipation unresponsive to fiber, hydration, and lifestyle changes may require prescription intervention. Osmotic laxatives like polyethylene glycol (MiraLAX) are generally safe for regular use and may be appropriate for some GLP-1 users as part of their treatment protocol.
Discuss persistent digestive issues with your prescribing physician. Severe gastrointestinal side effects occasionally necessitate dose adjustment or switching to a different GLP-1 formulation.
The microbiome perspective
Your gut microbiome undergoes significant shifts during rapid weight loss and dietary change. The bacteria that thrived on your previous diet may decline as substrate availability changes. New populations emerge to fill the altered ecological niche.
Fiber serves as the primary fuel source for beneficial gut bacteria. Adequate fiber intake during GLP-1 therapy supports microbiome diversity and the production of short-chain fatty acids that nourish intestinal cells and reduce inflammation.
Conversely, very low fiber intake allows less desirable bacterial populations to expand. Some of these produce gases and metabolites that contribute to bloating, discomfort, and irregular bowel function.
Viewing fiber as food for your gut bacteria, rather than simply bulk for your stool, reframes its importance. You are not just feeding yourself. You are feeding an ecosystem that profoundly influences your digestive comfort, immune function, and potentially even your mood.
Fitting fiber into your glp-1 nutrition strategy
Gut health interconnects with every other aspect of nutrition during GLP-1 therapy. Adequate fiber supports the absorption of micronutrients covered in our article on vitamin deficiencies and weight loss drugs. It complements protein intake by promoting the gut environment where amino acids are absorbed. It works synergistically with hydration strategies.
For the complete picture of how these nutritional elements work together, our comprehensive guide to GLP-1 nutrition provides an integrated framework.
Digestive discomfort does not have to define your GLP-1 experience. With strategic fiber intake and attention to the factors that support gut health, most users find significant relief. What changes have you made to your fiber intake since starting GLP-1 therapy, and what has worked best for you?