The frustration is real. You know what you should eat. You understand that processed snacks are doing you no favors. Yet every time you try to “eat clean,” something pulls you back to the drive-thru, the vending machine, the late-night pantry raid. What most people don’t realize is that this isn’t a willpower problem. It’s a neurobiology problem. And in 2026, science finally has enough evidence to explain why dietary transformation requires a fundamentally different approach than simply “eating better.”
Research from Drexel University’s Center for Weight, Eating, and Lifestyle Science has documented what clinicians now call ultra-processed food addiction, or UPFA, affecting roughly 14% of adults and 15% of youth globally. This isn’t metaphorical addiction. Brain imaging studies reveal that repeated consumption of hyperpalatable foods, those engineered combinations of sugar, fat, and salt, triggers the same dopamine pathway alterations seen in substance use disorders. The reward system becomes desensitized. The brain demands more stimulation to feel the same pleasure. Cravings intensify while satisfaction diminishes.
Understanding this neurological reality isn’t meant to excuse poor eating habits. It’s meant to inform strategy. Because willpower alone, it turns out, is the weakest predictor of successful dietary change.
Why the kitchen matters more than the gym
Before diving into what to eat, consider where you eat. Data from the University of Washington’s Center for Public Health Nutrition reveals a striking pattern: people who cook at home six to seven times per week consume significantly fewer calories, less sugar, and less fat than those who cook infrequently, even without consciously trying to diet. The effect persists when these frequent home cooks occasionally eat out. They still make better choices.
A separate population-based cohort study of over 11,000 UK adults found that consuming home-cooked meals at the highest frequency correlated with better scores on both the Mediterranean Diet Score and the DASH score, two gold-standard measures of diet quality. Participants also showed lower body fat percentage and more favorable metabolic markers.
The mechanism is straightforward. Home cooking puts you in control of ingredients, portions, and preparation methods. Restaurants, even upscale ones, routinely add several tablespoons of butter or fat per dish because it makes food taste better. When you cook at home, you decide whether that fat goes in.
The financial argument works too. Research consistently shows that home-cooked meals cost less per serving than eating out, roughly $4.31 versus $20.37 on average. Restaurant food prices have been climbing faster than grocery costs, widening that gap every year.
The fiber foundation you’re already building
Here’s encouraging news for anyone already targeting 25 grams of fiber daily: you’re ahead of 97% of Americans. According to the U.S. Department of Agriculture, almost the entire population fails to meet the recommended fiber intake of 25 to 34 grams per day. The typical American diet hovers around 15 grams.
But fiber isn’t just about bowel regularity, the original basis for intake recommendations decades ago. A UC Irvine intervention study found that participants who increased their fiber intake by 25 grams daily for just two weeks experienced measurable shifts in their gut microbiome, including increased populations of beneficial bacteria like Bifidobacterium and Lactobacillus. These microbes produce short-chain fatty acids, metabolites that nourish intestinal cells, reduce inflammation, regulate immune responses, and may even influence gene expression related to cancer prevention.
The catch is that fiber diversity matters as much as quantity. Different gut bacteria specialize in breaking down different fiber sources. Someone who suddenly eats 25 grams of black beans without prior adaptation will likely experience gas and bloating because their gut lacks sufficient black-bean-digesting bacteria. The solution is gradual introduction of varied fiber sources: legumes, whole grains, fruits, vegetables, nuts, and seeds. One influential study found that eating more than 30 different types of plants each week correlated with higher gut microbial diversity.
The addition approach beats restriction
The psychology of dietary change has shifted significantly. Nutrition research in 2025 and 2026 increasingly emphasizes what clinicians call “crowding out” rather than “cutting out.”
When you focus on adding nutrient-dense foods, processed options naturally get displaced. Fill half your plate with colorful vegetables, and there’s simply less room for fries. Start lunch with a fiber-rich salad, and your appetite for the calorie-dense main course diminishes. This approach works because it doesn’t trigger the psychological reactance that comes with prohibition. Telling yourself you can’t have something makes you want it more. Telling yourself to add something feels like gaining, not losing.
A UCL clinical trial published in 2025 compared weight loss outcomes between participants eating nutritionally matched diets that differed only in processing level. The minimally processed food group lost nearly twice as much weight. Both groups followed dietary guidelines. The difference came down to how the food was prepared.
Practical architecture for change
The goal isn’t perfection. It’s consistent improvement that compounds over time. Here’s what evidence-based practice looks like:
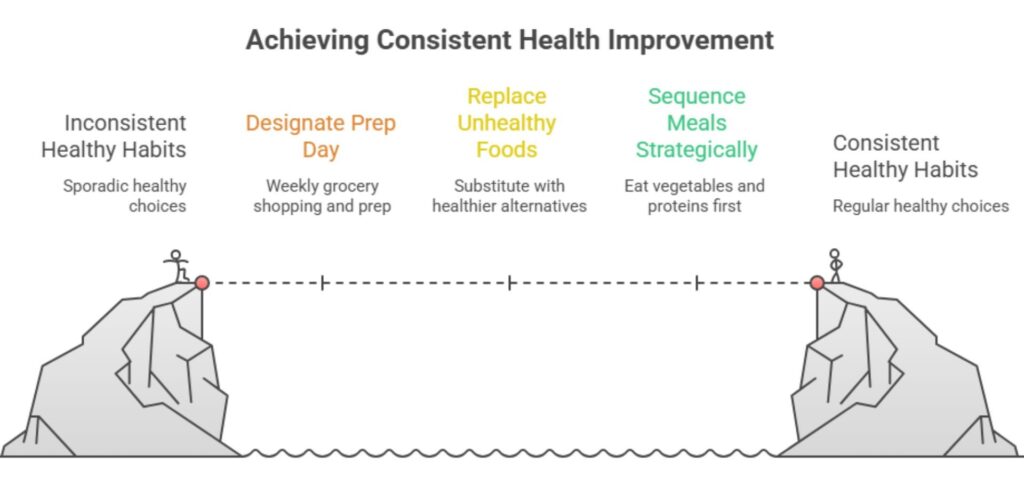
Designate a cooking prep day.
Choose one day weekly for grocery shopping and basic meal preparation. Wash and chop vegetables. Cook a batch of whole grains. Prepare lean proteins. This eliminates the friction that leads to “I don’t have time, let’s order takeout.”
Replace, don’t remove.
Craving chips? Try air-popped popcorn, a whole grain with decent fiber. Missing soda? Sparkling water with fruit infusion provides the fizz without the sugar. Want a burger? Make it at home with lean beef or turkey, controlling sodium and fat.
Sequence your meals.
Emerging research on meal sequencing suggests eating vegetables and proteins before starches may reduce post-meal glucose spikes and enhance satiety. This isn’t about restriction. It’s about strategic ordering.
Expect a recalibration period.
Taste preferences adapt. Studies show that reducing ultra-processed food consumption for two to three weeks begins resetting dopamine sensitivity. Foods that once seemed boring start tasting more satisfying. But this requires weathering an initial period where nothing seems as good as the hyperpalatable foods your brain remembers.
The processed meat question
Cutting out pork and processed meats, as many health-conscious eaters are doing, aligns with substantial epidemiological evidence. Processed meats contain preservatives, nitrites, and high sodium levels linked to increased colorectal cancer risk and cardiovascular disease. The World Health Organization classified processed meat as a Group 1 carcinogen, the same category as tobacco smoking, based on sufficient evidence of carcinogenicity in humans.
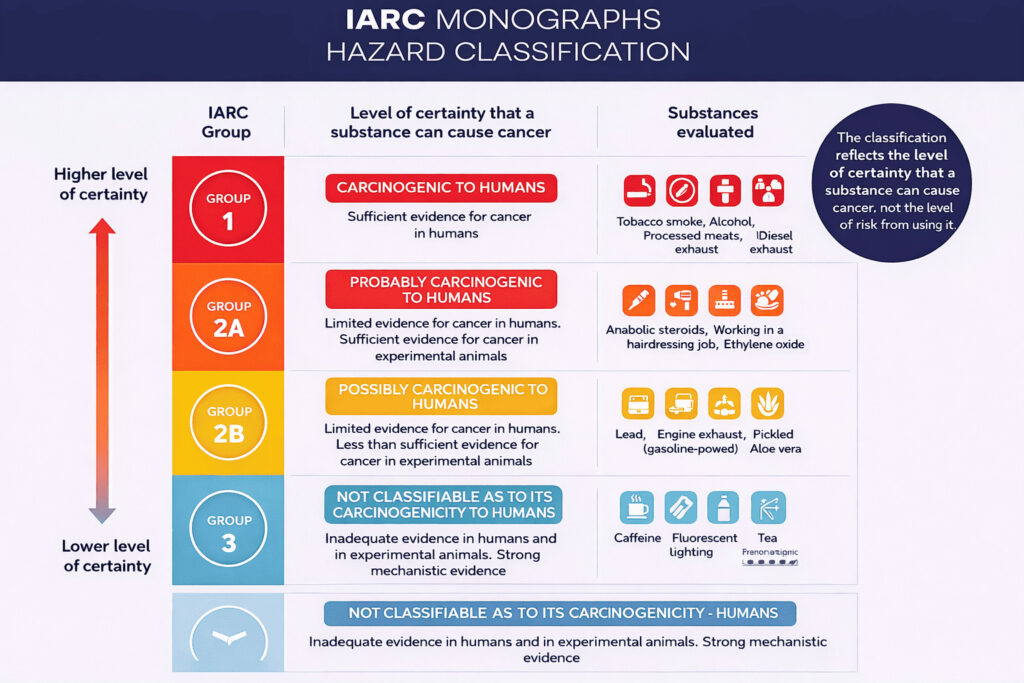
This doesn’t mean all meat is problematic. Unprocessed poultry, fish, and lean cuts of beef can fit within healthy dietary patterns. The issue is specifically with bacon, sausages, hot dogs, deli meats, and similar products that have been cured, smoked, or preserved.
What long-term changers actually do
A qualitative study published in the journal Health Psychology Open interviewed people who had successfully maintained significant dietary improvements for at least two years. Five themes emerged: a strong desire to feel better physically and mentally, extensive self-directed research and learning, development of helpful habits like meal planning and batch cooking, recognition of tangible benefits that reinforced the changes, and alignment with personal values.
Notably, only two participants had sought professional guidance during their transition. Most described a process of experimentation, reading, and gradual adjustment. They valued understanding the reasons behind recommendations rather than following prescriptions blindly.
This suggests that sustainable change emerges from intrinsic motivation and personal ownership. External rules imposed without understanding tend to collapse. Internal conviction built through learning tends to persist.
The bottom line
Changing a diet after years of unhealthy eating is neither quick nor easy, but it’s also not about superhuman willpower. The brain adaptations that make processed food feel irresistible can be reversed through consistent exposure to whole foods. The gut microbiome that may currently be optimized for junk can be reshaped within weeks through fiber diversity. The taste preferences that crave sugar and salt will recalibrate when given time.
Start with home cooking. Build fiber variety gradually. Focus on adding rather than subtracting. Expect discomfort during the transition and recognize it as evidence of neurological change, not personal weakness. The path isn’t dramatic transformation overnight. It’s small, sustainable shifts that accumulate into a fundamentally different relationship with food.
What specific food swap have you found most helpful in your own dietary transition?











