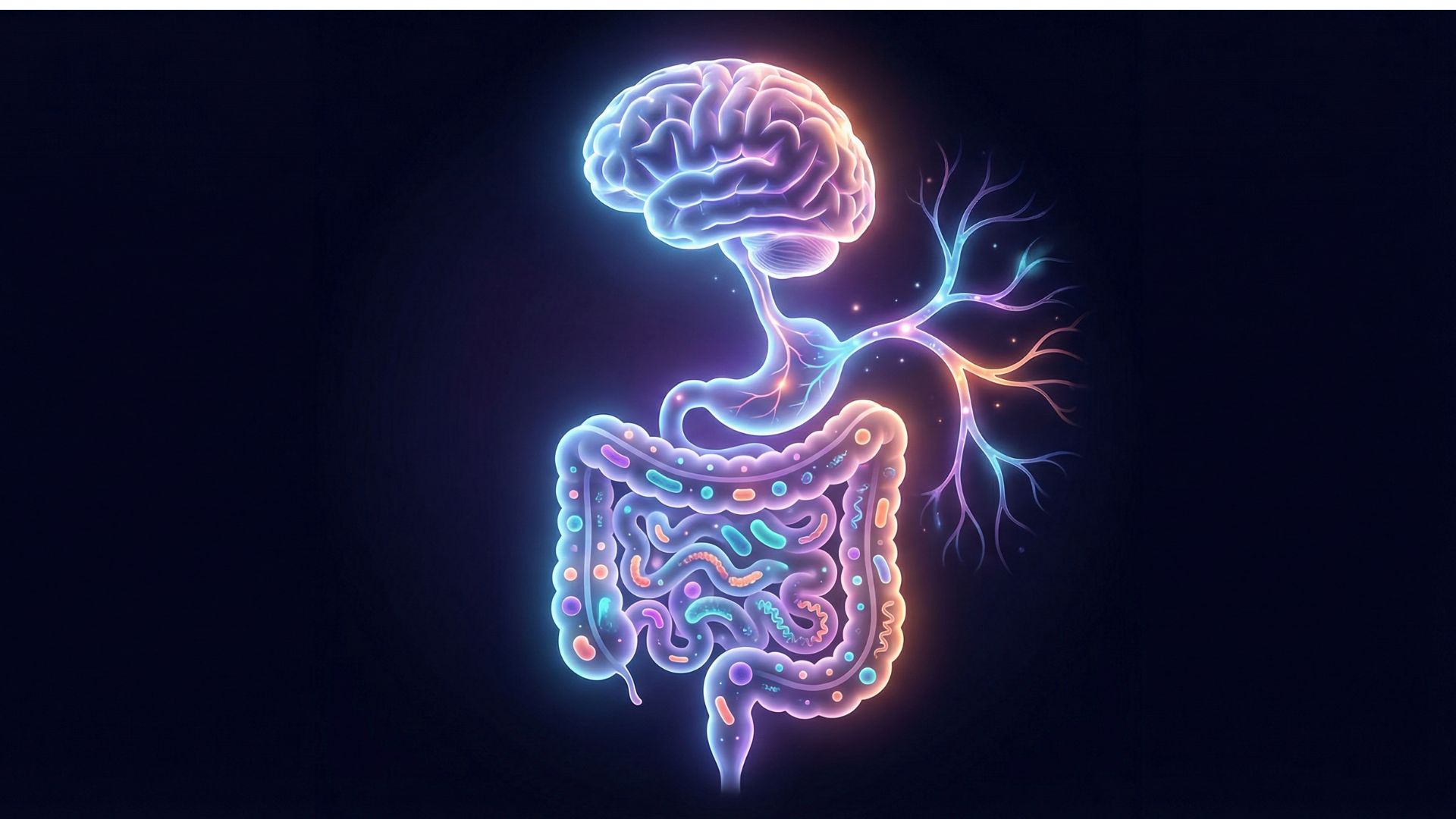
That persistent anxiety you’ve been feeling might have nothing to do with your workload or that upcoming presentation. Instead, the culprit could be lurking in your gut, where trillions of microbes are quietly orchestrating your emotional state through an intricate communication network scientists call the gut brain axis.
After spending two decades researching nutrition and traveling to remote communities where depression rates remain mysteriously low, I’ve become convinced that Western medicine has been looking for mental health solutions in all the wrong places. The answer isn’t always in our heads; sometimes it’s in our intestines. Understanding this connection is essential for anyone pursuing a complete guide to gut health optimization
The two-way street between your gut and brain
Your gut and brain maintain constant conversation through the vagus nerve, a superhighway of communication that runs both directions. When your gut microbiome becomes imbalanced, it sends distress signals upward that manifest as anxiety, brain fog, or depression. Conversely, chronic stress from your brain creates havoc below, disrupting the delicate bacterial ecosystem in your intestines.
This bidirectional relationship explains why so many people experience butterflies in their stomach when nervous or lose their appetite during emotional upheaval. Your gut literally has its own nervous system, often called the second brain, containing over 500 million neurons that operate independently yet communicate continuously with your primary brain.
Your gut: the neurotransmitter factory
Here’s what really blew my mind when I first discovered it during my doctoral research: your gut produces approximately 90% of your body’s serotonin. Let that sink in for a moment. The neurotransmitter most associated with happiness and wellbeing isn’t primarily manufactured in your brain but in your intestines.
Beyond serotonin, your gut microbes are busy producing dopamine, GABA, and dozens of other neurotransmitters that regulate everything from motivation to sleep quality. These microscopic chemists work around the clock, converting the food you eat into mood-altering compounds that directly influence how you think and feel.
The implications are staggering. Traditional approaches to mental health that ignore gut health are essentially treating symptoms while ignoring root causes. It’s like trying to fix a car’s performance issues without ever checking the engine.
When good bacteria go missing
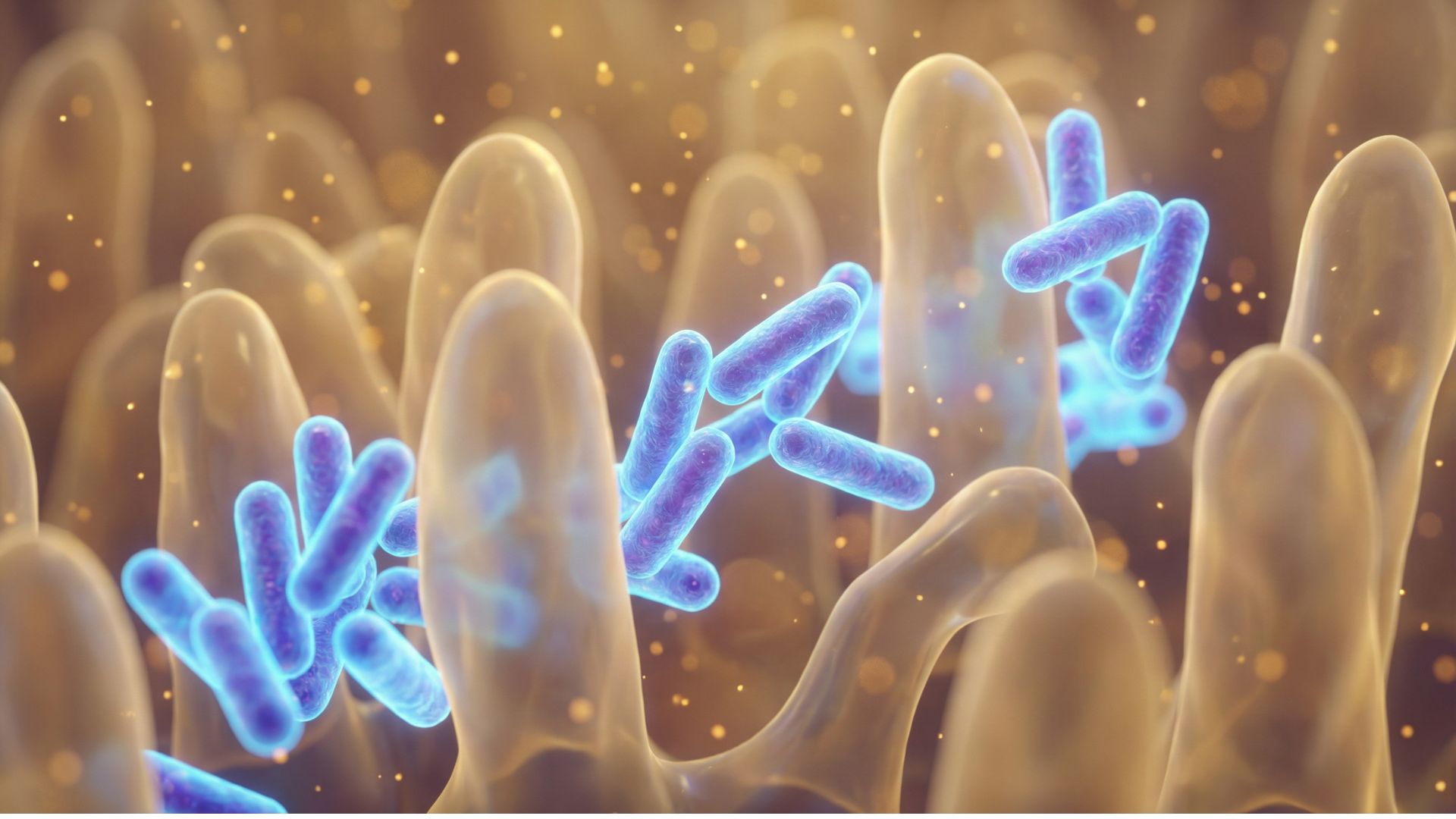
Modern life wages war on beneficial gut bacteria. Every course of antibiotics, every meal of processed food, every night of poor sleep diminishes your microbial allies. The herbicide glyphosate, present in conventionally grown foods, acts as an antibiotic in your gut, selectively killing beneficial bacteria while allowing pathogens to flourish.
When protective bacteria disappear, opportunistic pathogens migrate from the large intestine into the small intestine, a condition called small intestinal bacterial overgrowth or SIBO. These unwelcome guests produce toxins that cross the intestinal barrier and enter your bloodstream, triggering inflammation throughout your body and brain.
The research connecting gut dysbiosis to mental health conditions keeps piling up. Studies now link imbalanced gut bacteria to depression, anxiety, ADHD, autism spectrum disorders, schizophrenia, and even Alzheimer’s disease. In many cases, addressing the gut imbalance leads to remarkable improvements in mental symptoms that years of conventional treatment couldn’t achieve.
Your microbiome makes more than just serotonin
While humans produce only 17 digestive enzymes, your microbiome manufactures over 60. These bacterial enzymes don’t just help you digest food; they transform nutrients into bioactive compounds that influence your brain chemistry. For instance, certain bacteria convert dietary fiber into butyric acid, a compound that mimics ketones and provides direct fuel for brain cells.
Your gut bacteria also produce vitamins, particularly B vitamins crucial for mental health. They manufacture vitamin K, essential for blood clotting and bone health. They even create novel antioxidants from plant compounds that your human cells couldn’t produce alone.
Perhaps most remarkably, specific bacterial strains produce natural antibiotics that keep pathogenic bacteria in check without harming beneficial species. This natural defense system operates continuously, maintaining order in your intestinal ecosystem without the collateral damage of pharmaceutical antibiotics.
Signs your gut-brain axis needs attention
How do you know if your mental health struggles stem from gut imbalance? Watch for these telltale signs that often appear together: mood changes accompanied by digestive issues, brain fog after eating certain foods, anxiety that worsens with bloating, depression coupled with irregular bowel movements, or sleep problems combined with food sensitivities.
Many patients tell me they never connected their digestive symptoms with their mental health until we addressed both simultaneously. The relief they experience when we restore gut balance often surpasses years of conventional mental health treatment.
Rebuilding your mental health from the inside out
The good news is that your gut microbiome responds quickly to positive changes. Within days of improving your diet and lifestyle, beneficial bacteria begin to rebound. Within weeks, many people report significant improvements in mood, energy, and mental clarity.
Start by eliminating processed foods and adding fermented foods like sauerkraut, kefir, and kimchi to your daily routine. These living foods deliver beneficial bacteria along with the prebiotics that feed them. Consider targeted probiotic supplementation, particularly strains proven to support mental health. Create an environment where beneficial bacteria thrive through stress management, quality sleep, and regular exercise.
The path to mental wellness might not start in your head after all. By nurturing the microscopic ecosystem in your gut, you’re laying the foundation for emotional resilience that no amount of positive thinking alone could achieve. Understanding when to take probiotics for maximum effectiveness becomes crucial when you’re serious about optimizing this gut-brain connection.
What digestive symptoms have you noticed during times of stress or anxiety?